Patients want to be at home. As the only company to use data science-driven solutions, Medalogix transforms home health and hospice, enabling more patients to experience timelier, more responsive care where they are most comfortable.
Unlock
Data-Driven Care
Dedicated to empowering individualized patient care with innovative, data science-driven solutions that enable a shift to value-based care.
Medalogix Leverages State of The Art Machine Learning
At every step in the home health and hospice journey, Medalogix brings transparency through its solutions. Clinicians can quickly identify critical risks and key insights. More informed, more effective care decisions can help patients stay healthier longer – and that reduces rehospitalization.
The only all-in-one home health software solution that uses cutting-edge data science to bring EHR data to life, empowering clinicians and home health organizations alike to provide timely, evidence-based care for every patient.
Pulse is Expanding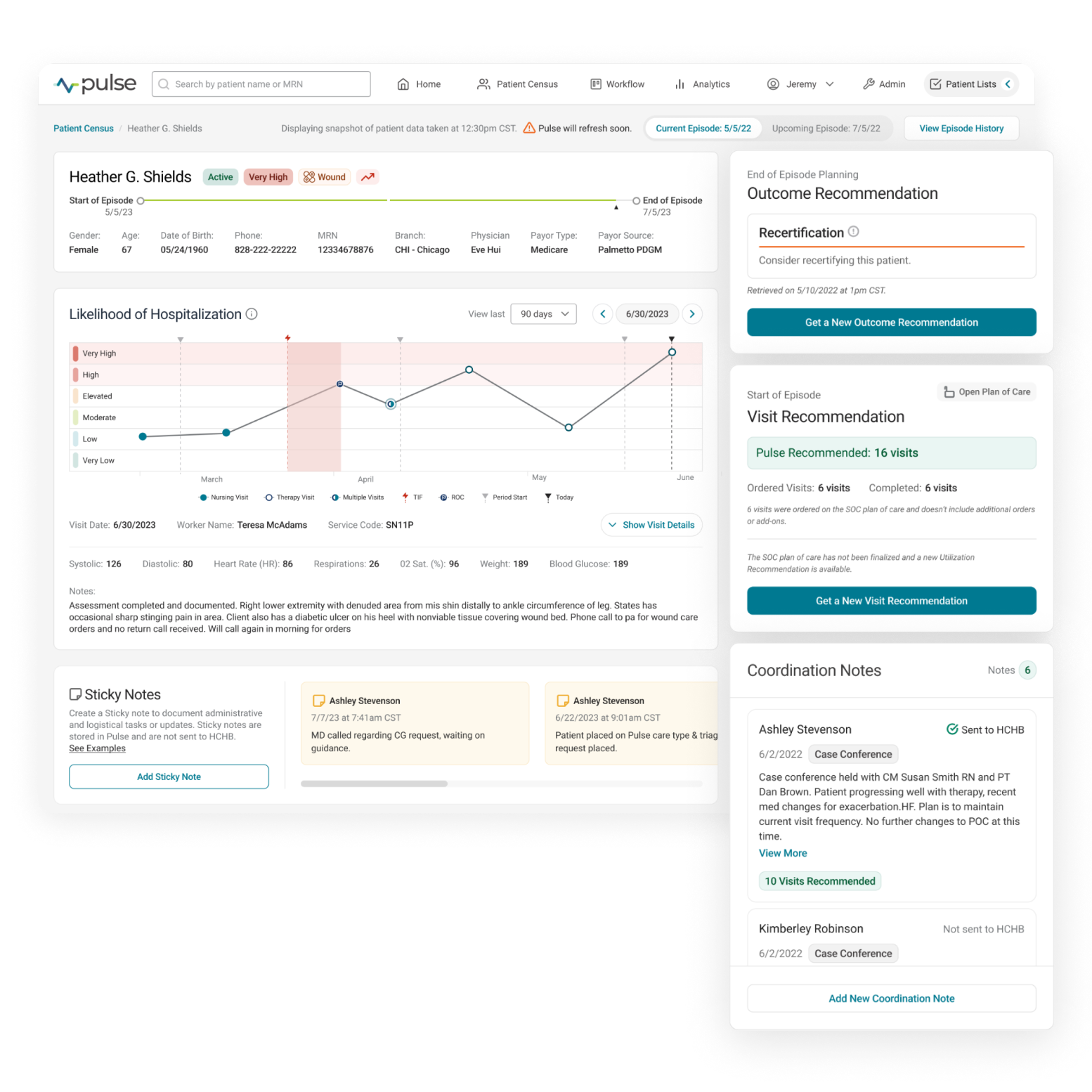
Home Is Where the Health Is
Right Care, Right Time
Backed by data science and built with clinical expertise, Medalogix is at the center of healthcare’s shift towards value-based care with a focus on reducing the risk of hospitalization. We support agencies caring for over 30% of the U.S. home health population and 20% of the hospice population. Medalogix solutions enable unprecedented visibility, transparency, and coordination. We give you the most complete, data-driven view possible into the patient trajectory.
End-of-life Planning
Identifies Home Health patients that may benefit from end-of-life care.
Explore Bridge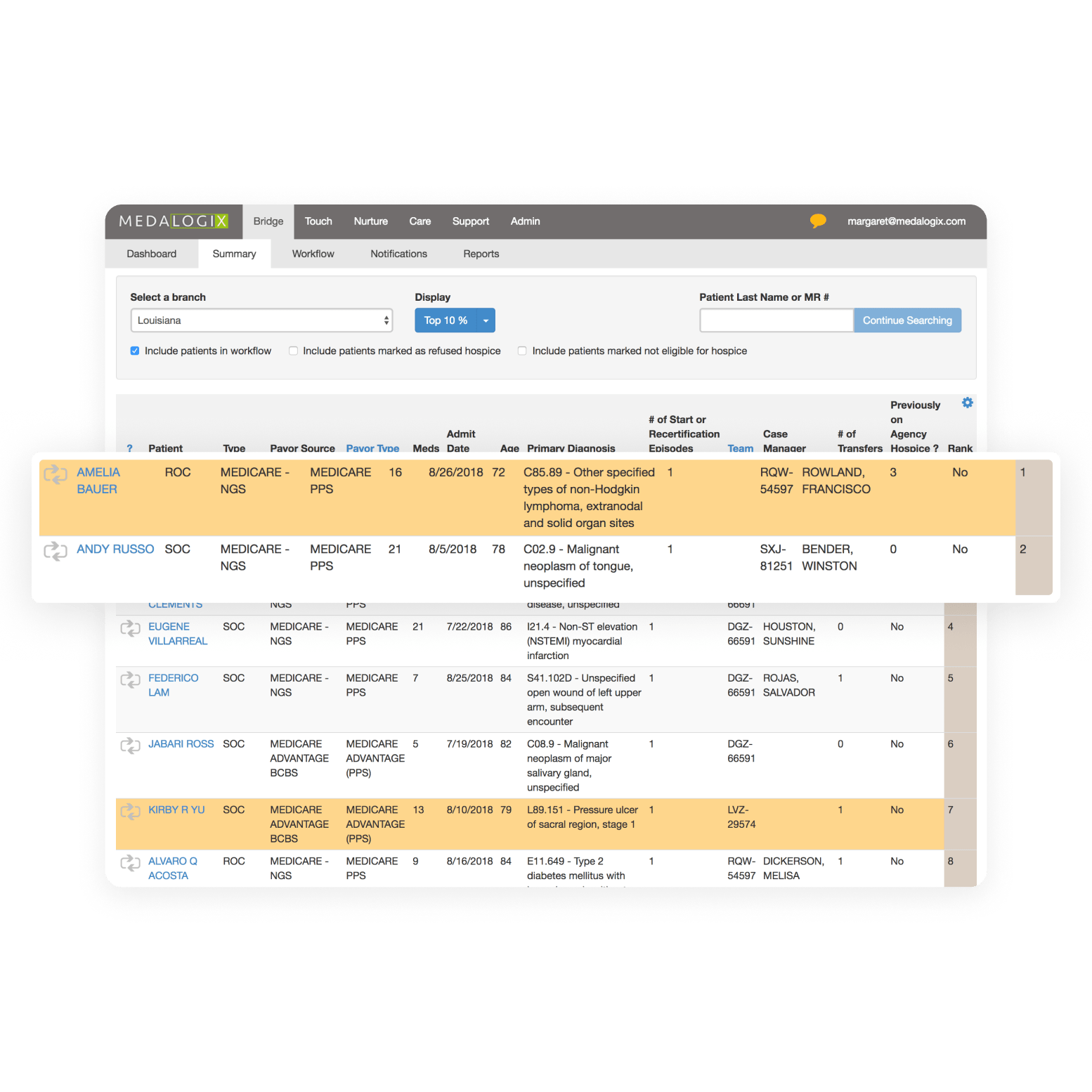
Hospice Care Utilization
Predicts hospice patient transitions to enable optimal end-of-life care.
Explore Muse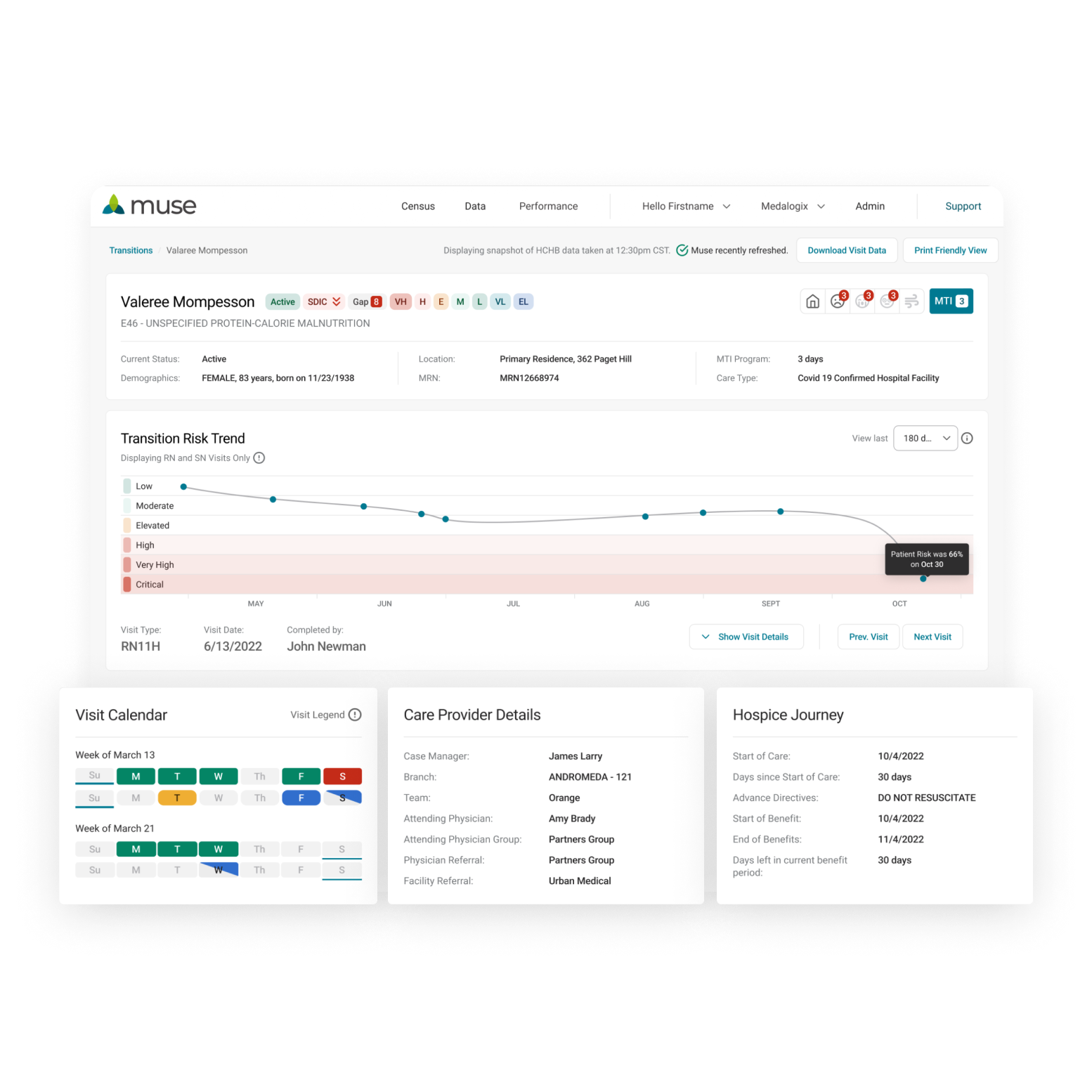
The Medalogix Difference
Featured In





Our Expertise

Announces Release of Pulse Referrals & Admissions Modules Backed by Generative AI
Pulse modernizes admissions workflows with proprietary documentation imp…

Improving Hospice Care with Data-Driven Insights: A Conversation with Knute Nelson Hospice
Providing compassionate and high-quality support to patients and their f…

The FY 2024 Hospice Payment Rate Update Proposed Rule: Why Quality Matters Even More
By: Cyndi Rizzitello, MSN, RN, BC On March 31, 2023, the Centers …

Unlocking Efficiency and Precision in Home Health Documentation
Home health teams operate in diverse and uncontrolled settings, ranging …

High-quality, accessible data essential to strong home health practices and outcomes
When it comes to providing quality home health care, agencies are only a…

Pulse Referrals & Admissions: A Q&A with Medalogix President and CEO Elliott Wood
With our new Referrals & Admissions module now available for purchas…
